CONDITIONS EXPLAINEDHerniated Discs
CONDITIONS EXPLAINEDHerniated Discs
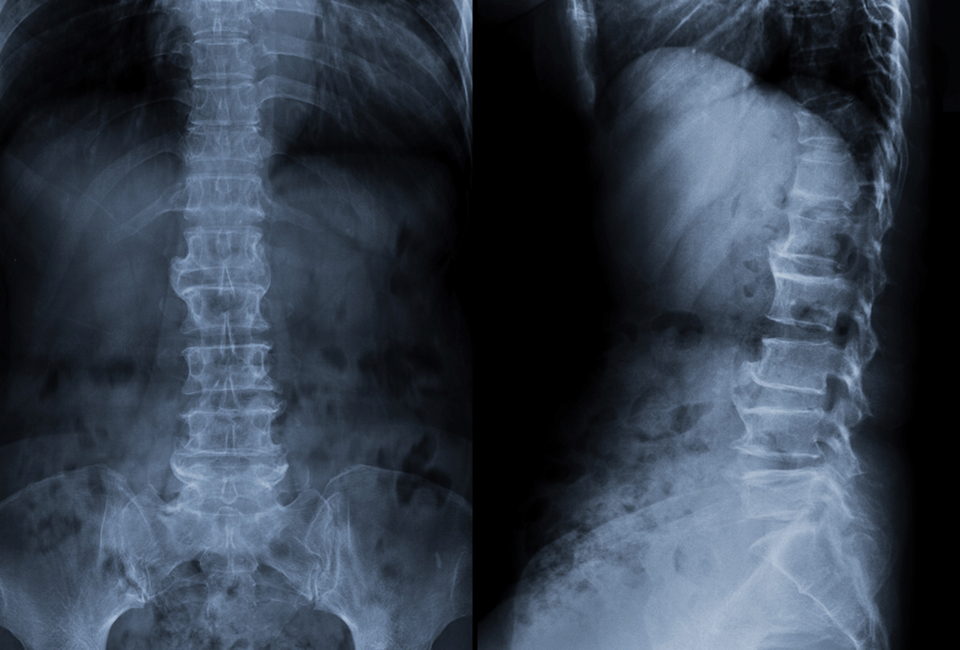
Herniated Discs are an extremely common condition affecting the cushioning discs that lie between each vertebra in the spinal column. The discs are composed of a fibrous outer coating, and a gel-like inner nucleus. With injury or degeneration, the soft nucleus can bulge out from its fibrous capsule and compress local structures, as well as releasing potent inflammatory mediators that further compound the pressure on surrounding structures. This often painful condition can impinge on the spinal cord and nerve roots traveling out from it, causing numbness, weakness, and pain in associated regions. Pain typically only affects one side of the body.
There are many causes for disc herniation, some of the most common including simple wear and tear, repetitive movements, improperly lifting, trauma, obesity, and genetic factors. In addition, the discs lose fluid over time becoming more rigid. This leads to greater susceptibility to injury as they become weaker and more brittle. Generally, care should be taken to avoid placing the brunt of a load onto the back. Injury can occur across a range of severities, and symptomatic presentation is different in most instances.
The symptoms of disc herniation vary between individuals, but the most common include:
- Pain ranging from a dull ache to sharp severity
- Numbness, burning, and tingling like the sensation of pins and needles
- Muscle Weakness, numbness, with the potential for altered reflexes and spasticity.
- Loss of bowel or bladder control in extreme cases – Requires immediate medical evaluation
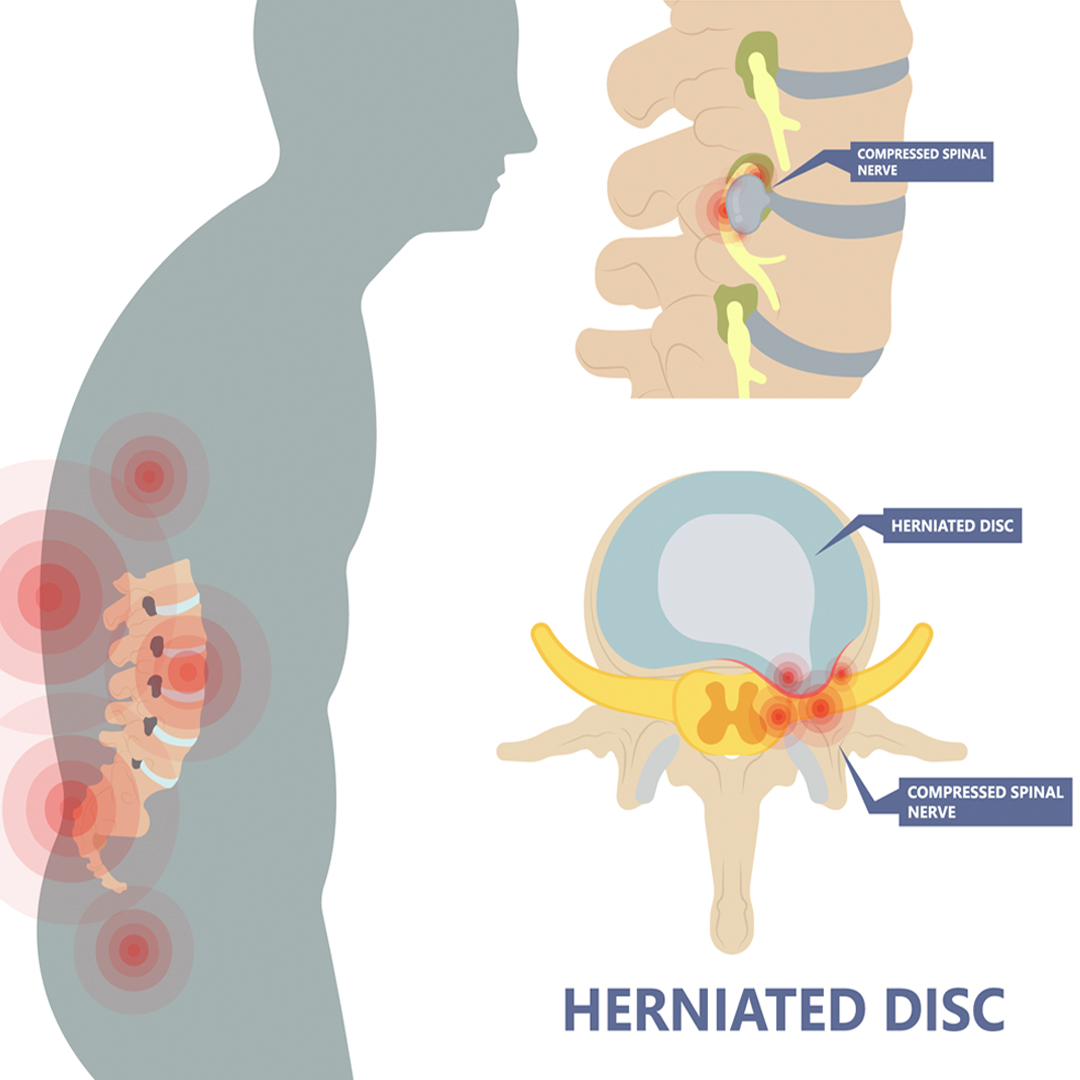
Herniated Discs are an extremely common condition affecting the cushioning discs that lie between each vertebra in the spinal column. The discs are composed of a fibrous outer coating, and a gel-like inner nucleus. With injury or degeneration, the soft nucleus can bulge out from its fibrous capsule and compress local structures, as well as releasing potent inflammatory mediators that further compound the pressure on surrounding structures. This often painful condition can impinge on the spinal cord and nerve roots traveling out from it, causing numbness, weakness, and pain in associated regions. Pain typically only affects one side of the body.
There are many causes for disc herniation, some of the most common including simple wear and tear, repetitive movements, improperly lifting, trauma, obesity, and genetic factors. In addition, the discs lose fluid over time becoming more rigid. This leads to greater susceptibility to injury as they become weaker and more brittle. Generally, care should be taken to avoid placing the brunt of a load onto the back. Injury can occur across a range of severities, and symptomatic presentation is different in most instances.
The symptoms of disc herniation vary between individuals, but the most common include:
- Pain ranging from a dull ache to sharp severity
- Numbness, burning, and tingling like the sensation of pins and needles
- Muscle Weakness, numbness, with the potential for altered reflexes and spasticity.
- Loss of bowel or bladder control in extreme cases – Requires immediate medical evaluation

Patient Animation VideoHerniated Discs
Experiencing Symptoms of Herniated Discs?
Detection & Diagnosis
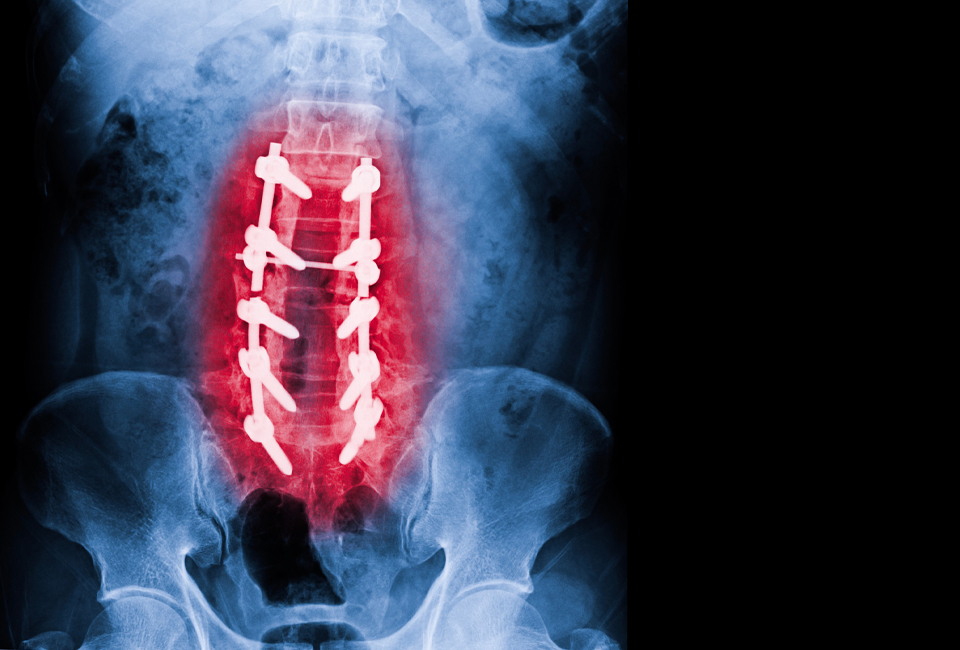
Physical examination can do much to identify the cause of back problems, and x-rays are routinely ordered examining the back. Unfortunately, x-rays do not provide good visualization of softer tissues such as the vertebral discs, and usually cannot definitely diagnose this condition. As such, more useful diagnostic modalities include: